Public Health Spending in India: Is 1.3% Enough?
The healthcare system in India is in a massive transition. The nation has evidently achieved over the last ten years growth in access to healthcare, and increase in key health metrics as well as the introduction of massive programmes like Ayushman Bharat. These initiatives have assisted millions of people to receive healthcare services which were not available before.
But the question lurking below these gains is one that still continues to feature in policy discussions; Is India spending on its people enough on health? The problem is not only the sufficiency of the funding since the government health expenditure is around 1.3%-1.9% of GDP. It is concerning the national agenda, the promise of equity and readiness to address the upcoming health challenges.
The question of the spending of public health becomes even more acute because India is looking forward to having Universal Health Coverage (UHC). Could such a healthcare system be robust and inclusive in a nation with more than 1.4 billion individuals with such a low investment in it?
Examining India Health Spending Terrain.
The public expenditure in India has been rising progressively in terms of health expenditure however at a rather slow rate. According to government statistics, over the past few years, the public health expenditure has already reached nearly 1.9 percent of the GDP. Although this is a good development, it is still very low compared to the rest of the world.
In most developed nations, the government expenditure on health is higher than 6-7 percent of GDP. The averageis much greater than the one in India even among the developing economies, and BRICS nations. This disparity underscores a basic issue that the health system of India is likely to recommend a very high and varied population with arelatively low number of financial resources.
It is not only the question of the amount of money spent, but the effective use of the available means as well. Inadequate finances tend to create discontinuities in infrastructure, employment, and lapses in service provision particularly in rough areas and underserved areas.
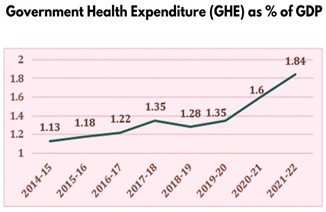
A Historical Approach: Stagnant Underinvestment.
The low level of expenditure on public health in India is not an eventual occurrence. In the previous decades, the government used to spend between 1% and 1.2% of the GDP on health. This was the level of investment that put India at low position in the world in terms of spending on health in a public way.
Upon realizing this gap, the National Health Policy (2017) established a goal of 2.5 percent of GDP by which it aims to raise expenditure on the public health. The policy noted the need to enhancethe primary healthcare, minimise the out-of-pocket spending, and enhance access to quality services.
Although this is promised, the pace towards the target has been very sluggish. Although the spending has been gradually increasing, it has not been enough to service the rising needs of the population. The disconnect between policy objectives and reality in terms of spending remains a limiting factor to the effectiveness of health interventions.
A Burden on Households: High Expenditure Out of Pocket.
Out-of-pocket expenditure in India is one of the greatest results of low expenditure on health by the populace. Households finance a high share of healthcare expenses and thus it can cause financial distress.
To most families, even one hospitalization can leave them with a debt of high proportions or even belowthe poverty line. This is especially so to vulnerable populations such as the people in rural areas and in the informal sectors.
The government has tried to solve this problem by government programs like Ayushman Bharat which have been taken to offer financial cushions to secondary and tertiary care. Nonetheless, there isstill limited public expenditure that implies that coverage is a partial one with many services that cannot be availed to every person.
The abatement of out-of-pocket spending needs not only to enlarge insurance schemes but also to reinforce the infrastructure and services of the public healthcare.
Disparity in Access: The Rural-Urban Dilemma.
The allocation of healthcare services to the regions is also determined by public health spending. In India, there is awide disparity in the accessibility of healthcare in urban and rural areas.
Cities are more likely to be better equipped in terms of infrastructure, more clinics, and medical practitioners. Conversely, the rural setups are usually hit by the lack of doctors, nurses andeven medical supplies.
Primary Health Centres (PHCs) which are supposed to be the first point of contact by the rural folk are often faced by the lack of resources and staffing. This restricts their capacity to offer good and prompt care.
This has led to the large number of people utilizing the services of privately-owned healthcare providers despite the high-cost involved. This gives a structure in which quality healthcare access is tightly tied to income, which supports existing disparities.
Lessons of the COVID-19: a Stress Test of the System.
The COVID 19 pandemic revealed both the advantages and disadvantages of the healthcare system in India. Although the nation showed its resiliency and innovation in some aspects, it also showed some extensive infrastructure, workforce potential and emergency response gaps.
Bed, oxygen and critical equipment shortage were experienced in hospitals during peak waves. It was hard to control the magnitude of the crisis using the available resources of the public health systems, and it was necessary to invest more in health infrastructure.
Despite the fact that the pandemic led to higher government expenditures, the growth was mostly temporary. The experience highlighted the need to maintain long-term investment in the health of the population to develop a system that can respond to a disaster in the future.
Indications of Improvement: Good Things.
Though, with the difficulties there have been significant changes in the public health scenario in India. There is an increase in government health spending at absolute rates and the proportion of government expenditure of the total health expenditure has also been enhanced.
The programs like the Ayushman Bharat have increased the coverage of healthcare services, especially to the poor segments of the population. Efforts aimed at enhancing the digital health systems, like Ayushman Bharat Digital Mission, have also proven to enhance efficiency and coordination.
Also, there has been an extension of healthcare network through investments in infrastructure, including the new medical colleges and health facilities. Nevertheless, these are improvements that have to be accumulated and maintained in the long run.
Efficiency and Governance: Counting Spending.
Raising the public health expenditure is required, but not enough in itself. The success of expenditure is based on the management and utilization of the resources.
The implementation mechanisms, weak fund disbursement delays, and the poor coordination between the central and state governments are some issues that tend to reduce the effectiveness of investments.
Enhancement of the governance systems,transparency and accountability are important in ensuring that money isutilized efficiently. Monitoring and evaluation systems are important to monitor the progress and to determine ways of improvement.
The Preventive Care Gap.
The healthcare system in India has been more curative rather than preventive-based. This method is expensive and can be considered rather reactive, which means that health problems are only solved once they have occurred.
Preventive healthcare is one of the areas that can contribute to better results and lessen expenses in the long run. Immunization, nutrition programs, early diagnosis and health awareness programs, among other services should be provided to enhance the health of the population.
This shift is pegged on strengthening primary healthcare systems. Proper primary care network will lighten the burdenon the higher-level facilities and also make sure that the problems in the health are dealt with at an early stage.
Comparisons around the World Learning.
The countries who have been effective in approaches towards the attainment of Universal Health Coverage are the ones who have a greater portion of their GDP on the state health. It has been indicated that it may take the allocation of at least 5 percent of the GDP to extend inclusive and even-handed healthcare services.
The current level of expenditure in India is way below this level. This complicates the attainment of UHC objectives and the provision of solutions to new health issues like non-communicable diseases, old age and environmental health hazards. The experience of other countries can enable India develop a more efficient health financing policy and enhance the services delivery.
The Way Forward: Spurring More Investment and Enhancing Systems.
To over come these issues, India needs to make huge investments in health. This involves increment in the funding of primary health care, infrastructure, and health workforce.
It is also essential to enhance the governance, monitoring, and accountability systems. Resource utilization can be effective to increase the effectiveness of investments and service delivery. Access and efficiency can be further enhanced by investing in digital health, telemedicine and data systems, especially in remote and underserved locations.
Conclusion.
Whether 1.3 percent suffices or not is not merely a matter of statistics. It shows the health and well-being interest of the country towards its population.
Although over time India has achieved a breakthrough in increasing the availability of healthcare, the present amounts of government expenditure cannot be used to satisfy the increasing needs of the population. Bringing Global Health Coverage will need more funding as well as structural changes.
It is not only a social responsibility to invest in the health of the people in the long run. It is a need of the economy that promotes productivity, minimizes in equality, and promotes sustainable development.
The future health results of India will be based on the level at which it is taking this issue seriously.
References
1. https://www.pib.gov.in/PressReleasePage.aspx?PRID=203493
- https://www.pib.gov.in/PressReleasePage.aspx?PRID=2097868
- https://www.drishtiias.com/daily-updates/daily-news-analysis/indias-low-public-health-spending
- https://www.indiaspend.com/health/health-budget-grows-every-year-so-why-isnt-public-healthcare-improving-978653
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11633271/









